Recipient of the 2003 Clarion Award for Health Care Journalism and the Cystic Fibrosis Foundation’s Angel of Awareness Award

On February 21, 2003, I went to Laura Rothenberg’s apartment so I could see cystic fibrosis, but it turned out that if I was going anywhere near Laura Rothenberg, I would end up seeing Laura herself. Some people become their illness, and some deny or hide from their illness, but Laura had made the rare discovery of a way to contain her illness, as though she and it were roommates in her body. I’d been warned that she was nearly dead and wouldn’t be able to talk much, and on that first day, she was heavily drugged and could barely keep her eyes open. At 5’7″, she was down to below 90 pounds; she was breathing through an oxygen mask. I was unprepared for how she would battle against the ravages of her disease to make herself heard, for what a compelling personality she had preserved. I was a stranger intruding in the world of her final illness. But she knew that I would help give permanent evidence of her, and she wanted that very much.
Laura was dying at age 22. Aside from wartime heroes and film-star beauties, the people remembered best are those who achieve a lifetime’s accomplishments. Laura feared that her brief and fragile stay on earth might fade fast, so she lived an accelerated life, packing in experience because there wouldn’t be time to accrue it at a normal pace and always keeping meticulous records. When I met her, the evidence of that record-keeping was everywhere: in the years of tapes she had recorded, some of which had been edited into a National Public Radio program, “My So-Called Lungs”; in the numerous photos scattered around the house of every stage of her development; in journals and e-mails; in the big jar that contained every one of her hospital bracelets, from earliest childhood on; and most of all, in her remarkable, terrifying memoir, Breathing for a Living, which she wouldn’t live to see published.
“I’ve had to live all my life with the inability to known what’s going to happen next,” Laura said to me early on. “Which I have a lot of trouble with. I come back to it and back to it, just how hard it is for me to understand or deal with not knowing what’s going to happen in the future – except that I’m getting sicker.” It was a tragic statement, but from Laura it seemed matter-of-fact. Two years earlier, she’d made the decision to have a lung transplant. It was a risky procedure that could potentially extend her life but also could add more medical problems to the ones caused by cystic fibrosis; it could even kill her. “I was so careful,” she said. “I did everything I was supposed to do, but it didn’t work out for me. To go for it, to have the transplant, I had to think it would last 10 years. I don’t think I could have done it if I’d known it would be so brief. I had to get in gear for it, like some kind of marathon. But do I regret it? Oh, not given the time it bought me, the happiness.”
Cystic fibrosis (CF) is an incurable genetic illness that currently affects one in every 3,000 Caucasian newborns in the United States – the rates are much lower in nonwhite populations – for a total of about 30,000 Americans. People with CF have an average life span of about 30 years. The disease affects the glands that prodcue mucus, sweat, tears and other fluids in the body; instead of secreting the thin mucus that ordinarily coats the lungs, liver, pancreas and digestive tract, these glands generate a thick, sticky mucus that impedes function. The mucus renders the lungs more vulnerable to infection; it blocks the normal flow of pancreatic juices, preventing the body from digesting and absorbing fats and fat-soluble vitamins, which leads to malnutrition and poor weight gain. Though symptoms vary from person to person, an average CF patient can have episodes of acute intestinal pain and cramps, as well as clogged airways that make breathing difficult and can cause a persistent, violent cough. CF sufferers are also at risk for diabetes, gallbladder infections, cirrhosis and infertility.
Laura had “everything that cystic fibrosis can offer,” one of her doctors, Celia N. Ores, M.D., told me. “She got a full plate. She had sinus disease; she had progressive lung disease; she had intestinal problems – and then some. Cystic fibrosis is a very unkind disease, and I would say it was particularly unkind to Laura.”

Laura Rothenberg at age six, before the worst symptoms of cystic fibrosis had set in.
Laura was diagnosed with CF when she was three days old, but she did relatively well during her childhood years. Still, by age five she had developed one of her disease’s early, debilitating symptoms: acute arthritis in her knees. “Big, swollen knees,” her father, Jon Rothenberg, M.D., said. “I remember taking her out to the school bus. And I was just brought to tears. She was pulling herself up on the bus – obviously in pain.” This was one of the first symptoms Laura’s classmates from The Chapin School, the rigorous New York City girls’ school she attended for 12 years, could see. “We went to a birthday party in a town house,” recalled one of Laura’s oldest friends, Elizabeth Grant, who goes by Eli. “She couldn’t run down the stairs with everyone else. She took them one at a time. I was just five myself, but I remember that as the first moment I understood she was really ill.” When Laura was in first grade, another Chapin student with CF passed away. “I suddenly understood that she had died,” Laura remembered, “and that if I had the same illness she did, that meant I would die too.”
She was determined to grab on to life in the time she had left, and she hatched a personality that brooked no contradictions. One day, I went to her spacious loft in downtown Manhattan while struggling with the tail end of bronchitis. Coughing in front of Laura was like playing ball in front of Michael Jordan, and she gave me tips. “You want to cough now,” she said. “Stop holding back that tickle in your throat. Just let it out – if you hold it back, it makes it 10 times worse, I’m telling you.” Laura was given to such frankness. She was outspoken, sometime outrageous, a little bit spoiled, a little bit spectacular, a natural leader; authoritative even in fields about which she knew little, autocratic but always, most of all, present in a heartbeat for anyone who needed her. Eli, who remembers going into the bathroom with Laura when they were children to admire her scars from postnatal intestinal surgery, explained, “She couldn’t be normal, so she had a choice. Rather than have everyone pity her, she chose to be someone special, a princess and a diva so everyone paid attention to her and respected her. She was bossy in a way that shut out sympathy. She didn’t want to be weak and at the receiving end of others’ generosity, so she was super strong and generous instead.” She set high standards, and sometimes it was a challenge for her friends to meet those standards. But they were encouraged to do so by how rigorously Laura herself rose to every occasion. Her passion for friendship took on almost mythological status. “For me, friendships are like falling in love,” she said.
One of her teachers said, “At our school, there was the official way, the unofficial way and the Laura way.” Part of the Laura way was to be the center of attention. Another Chapin teacher, Ann Klotz, said simply, “Laura was like royalty. Class was a court around her. The girls from her year thought smart was cool; she was right up there, and the kids she hung with were intelligent, hip and artsy. And she was so witty, funny. She was busy having a good time – she was a person who had a really good time despite everything and who gave others a good time too.” Laura had a wicked sense of humor that lasted through the latest stages of her illness. “I’m making up a list of people I’d like not to have at my memorial service,” she said to me one afternoon. “You can come.”
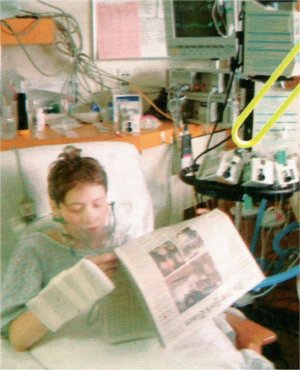
Laura Rothenberg after one of her many surgeries.
Starting around age 12, Laura spent much of her life in hospitals. “I’ve always felt happy and safe there,” she said. “In fact, I love it. We would sit up late at night, my hospital friends and I, and eat chocolates and champagne truffles and tell stories – it was an intimate place for me. I always had my Chapin friends or, later, my college friends who could understand some parts of me, but my CF friends were going through the same things, and they understood other parts of me.” She was popular at the hospital for her charm, and also because she was polite to and engaged with everyone who worked there, from doctors to maintenance staff. “If someone came to set up an IV, I said thank you. Not because I loved having IVs put in, but because they were doing their job, and they were doing their best, and it was supposed to help me. And a lot of them were shocked. They were used to people screaming and complaining, and this language of please and thank you took them by surprise.” She defied the anonymity of the sterile rooms by refitting them with her own pictures and possessions, including her trademark strings of origami cranes. What was inhuman, she humanized.
After Chapin, Laura went to Brown University; she chose it for its strong English department and the possibility that she could focus on creative writing and also because it was near an excellent children’s hospital where she could be treated in an emergency. Starting college was not easy. “I didn’t know what the procedure was for making new friends given how sick I was,” she explained; at the time, she wasn’t sure whether she had a year or a decade ahead of her. “My biggest mistake was to lay it on people before I knew I wanted to be friends with them – and if you do that, you don’t get very far.” During her freshman year, she found a running joke on a campus-wide chat site about “Coughing Girl.” Laura remembered entries such as “She’s back in all her wheezing splendor” and accounts of how many times she’d coughed during certain classes. “By that point, I thought I had established: ‘I’m Laura, and I have cystic fibrosis.’ But this made me feel like it was still, ‘I have cystic fibrosis, and I’m Laura.'” In The Brown Daily Herald, she wrote a scathing response: “At a school where differences are supposed to be respected and celebrated, I am appalled at the lack of compassion and understanding. Why should I have to disclose my private medical information? … I never asked to be the coughing girl … Think before you speak.” As her cough got worse, Laura had to defer to it more and more. “People would stare at me on the bus,” she told me. “Or at movies. It’s more trouble than you’d think.”
Balancing her isolating illness and her expansive personality was a constant and fierce battle, and Laura was prone to feeling alone – and abandoned. “A lot of the people at Brown were afraid,” she said, “and as I got sicker, people would stop calling or go away. One of my best, best, best friends, from freshman year – we were like to peas in a pod, Oreos and milk. But I think she couldn’t handle it. She decided not to room with me. I’ve been friends with dying people all my life, though, and I understand that it’s a big, hard commitment. I feel for the people who are my friends. I don’t want them to lose anything by knowing me.” Laura had lost dozens of hospital friends, many her own age, before she died herself. In a diary entry from 1997, she wrote, “I need a break, God, could you please not kill anyone else I know?”
Laura’s condition made her more reliant on her parents than others her age. She was close to both her mother and father. Mary’s love for her daughter was gentle and deep; Jon’s was passionate and complex. An internist who has worked mostly with disadvantaged populations, Jon is as brash, headstrong and assertive as Laura was – another huge personality, hypersensitized to the world’s challenges. His special hell was that he was one of the few people who fully understood Laura’s illness both as a medical reality and as a personal tragedy, and he spent decades increasing and concentrating his knowledge, yet was finally unable to save her. “I think there’s a colossal difference between being the parent of a child who has cancer and being the parent of a child with cystic fibrosis,” Laura told me. “There was no healthy period for me before CF set in. I’ve always been sick, and I don’t know how it would have been with my parents otherwise. Other people were fighting with their parents about how much TV they could watch, and I was arguing about taking my enzymes and doing chest PT [the tedious exercises CF patients are directed to do daily to clear their lungs]. I think that, somehow, they did a great job. Not like I’m the best person ever. Not that I was always the nicest person back to them – I certainly wasn’t. But they allowed me, at a certain point, to begin to take over. They balanced loving and respecting me.”
“You’d never know what liberty is until you met these parents,” Dr. Ores said. “They decided, very wisely, that to have Laura for a daughter was an extraordinary privilege and that her decision would always count. And in any case, Laura had to be persuaded to do what you wanted her to do. Unless she was convinced, she wouldn’t do it.” Laura’s relationship with her physicians, people who treat many sick and dying children, was unique. “She was never just a patient,” said Dr. Ores. “She immediately became something different. She was a friend, a colleague, a judge. Very giving, very intelligent, very judgmental. From early on, she asked many whys: Why this? Why that? And I liked this, immediately. I felt: You are dealing with someone who thinks for herself.”

Team Laura
Among the most difficult decisions Laura faced was whether to get a lung transplant. As one of her doctors said, “Transplantation involves exchanging one disease for another” – turning in the dying lungs for all the complications that come with the new pair. “I’ve had CF my whole life,” Laura wrote in her book. “I have a routine.” Getting the transplant meant “a new hospital, new doctors, new nurses, new faces and new rules… If I have a transplant, I can’t go back to life before the transplant… If I’m lonely, if I can’t go back to school as early as I hoped to, if I die…” It was not an easy choice. But it was her only chance at a longer life, perhaps as many as 10 more years.
And so in February 2001, during the second semester of her sophomore year, Laura took a leave from Brown and moved to Boston to wait for new lungs. Her friends threw her a lung retirement party; one made a poster that read: “Thank you to the lungs of Laura for 20 years of exemplary service.” Laura’s transplant surgery would be performed at Children’s Hospital Boston, and she would need to be ready at a moment’s notice when a pair of lungs became available. In her book, she describes sitting in a cafe one day and hearing a helicopter land some distance away: “Whenever I hear that noise, I think of my lungs arriving at the hospital. If I see a cooler in the park, I imagine my lungs inside of it.” She established a “transplant lottery” – she had all her friends propose dates when they thought the surgery would take place.
Everyone close to Laura was affected by her decision to have the surgery. Her father wasn’t working during this period; he wanted to spend as much time as he could with her and be there to help her through the surgery and recovery. “Going for the transplant,” said Laura, “was like going to have a baby. We had the transplant bag all packed and ready to go when the call came, and when it came and I went to the hospital, I felt as though a new life was being born, inside me, like a new life beginning.”
On July 15, 2001, Laura received the transplant. She documented and documented. Photos of the new lungs before they went in. Photos of the old lungs after they came out. These she framed and kept in her apartment, as though they were snapshots of friends. The doctors said that Laura would have had about six months to live based on how her old lungs looked. And the new lungs seemed like a success. For the first time in her adult life, Laura could breathe without effort. T-shirts were made for her friends and family: “Team Laura” on the front, and on the back, “The lungs have left the building.” The most poignant entries in her book and her radio diary are from right after the transplant. “That sound,” she says proudly on one recording, “those are my new lungs. I’m leaving the hospital after 19 days, and it’s very exciting. Most people ask, ‘How does it feel different to breathe?” and it’s funny, because it feels like a completely different body; everything about it seems new.” But that breathing was to be a very temporary release.
Within weeks of the transplant, Laura had a serious abdominal obstruction that required surgery. Then she developed a cancerlike condition that sometimes results from immunosuppressant drugs, which she needed to prevent her body from rejecting her new lungs. On immunosuppressants, you’re poised between rejection and infection: Too much of the medication and the body is vulnerable to opportunistic infection; too little and it will reject the lungs. She also developed stenoses, scars in the lungs that block the passage of air. So she would go under anesthesia almost every week for a bronchoscopy – or “bronch” – to break down the scar tissue. And then it would regrow and they’d have to go back in. Eventually, a specialist put in stents to keep the airways open, and another treatment eliminated the cancerlike condition. Laura had some 40 surgical procedures in the course of the 20 months her transplant held. She also had repeated pneumonia and a cascade of complications, including terrific gastrointestinal trouble and a worsening of her diabetes – “the cherry on the transplant sundae,” she called it.
Laura spent as much of the fall semester as she could at Brown – but by late October 2002, 15 months after the transplant, her doctors had told her there was little else they could do for her; by Thanksgiving, she was back home in New York. The transplant “was the first time I’d ever put complete faith in something,” she told me. “But every fear I had has come true. Sometimes I think about getting a second transplant, thinking, Well, it might be nice to live another two years. But I’ve had my chance.”

Laura and Bryan in February, six weeks before she died.
Ironically, love came to Laura in the last year of her life. Bryan Doerries – a smart, expansive 28-year-old theater director and poet who translates and stages Greek dramas – had been a counselor at a summer writing program Laura attended at the University of Virginia, and they had kept in touch when he was living on the West Coast. When he moved east, he e-mailed Laura, and they spent a rapturous day together. It was about six months after her transplant, and Laura was at a temporary zenith of strength. They walked around Bryan’s Brooklyn neighborhood for four hours and stayed up talking until 4 A.M. “I just had not context for her illness,” he said. “I was amazed at medical science, that I was walking around with a person who had had someone else’s lungs put in her body. She pulled up her shirt to show me, and her chest was covered in a latticework of scars. She wasn’t proud of it and she wsn’t ashamed – it just was.”
Bryan began to spend more time with Laura just as she was descending deeper into intractable illness. “I kept questioning myself,” he said. “Could I bear to be in love with someone so close to death? But in the end, it wasn’t up to me. I was in love with her. I didn’t give in right away, and I’m glad I didn’t – I really don’t think that if I had jumped in, I would have lasted through the end, that I would have had the endurance to make it through. Especially after the first time we made love, I was consumed by the lack of control I would have. I knew it would be like jumping off a cliff; there would be no fighting gravity from that point forward.”
On December 13, 2002, Laura and Bryan moved in together, though it was clear by then that she had only months left to live. “We were forced to try to live in the eternal present,” Bryan said. “But I could taste death with every kiss.”
Laura’s parents knew she wanted to experience a fragment of independent adulthood, and they went to great lengths to make Bryan feel welcome. “Mary was always deeply respectful of Laura’s wishes,” Bryan said. “Jon was very gracious in helping us to set up our adult life and giving her to me. You know, some fathers give their daughters to their husbands during a wedding procession. But the day he taught me how to do her pills was the day he gave me to Laura and Laura to me.”
As Laura’s illness progressed, so did Bryan’s role in her life. “My whole system became efficiently tuned to caring for her – how I slept, what I did, all my rhythms. I could be asleep through the entire night and wake up only when she needed help, and I’d know if she did, intuitively, from the way she was breathing.” In the very final weeks of Laura’s life, she achieved, at last, a calm and steady and mutual love. Bryan kept up her oxygen tanks and fed her and encouraged her, but more to the point, he simply loved her, listened to her, mitigated the aloneness in which her illness seemed to have trapped her. Laura gained all she wanted just as she lost all she had.
In our last conversation, Laura said to me, “I’ve been pretty lucky. I had the best medical help and lived a lot longer than most people could have hoped with my condition. I had the support of wonderful parents. I got to go to good schools. I had good friends. I got a book deal.” And then she paused and tilted her head toward the curtain between the bedroom and the living area, where Bryan was on the phone. “I even got to fall in love,” she said, and her voice lilted up with surprise. “I have a great boyfriend, and if I hadn’t had this year, I would never have found him. You can keep asking for more, but I’ve had a lot.”
And then, after a long silence, “Don’t get me wrong. I mean, I’m not stupid. For every one of those wonderful things, there was also something terrible. I call myself a positive realist. I am sad, deep down. I mourn, deep down, for what could have been. I got wise before my time. But I did get so much.”

Jon, Laura and May Rothenberg, Thanksgiving 2001.
Laura’s death, which Bryan described to me in careful detail, was something she controlled and created, consistent in this way with her life. The chronic rejection of her lungs was advanced; she could hardly get out of bed and was on so much pain medication that she was in a kind of trance most of the time. She set herself a final milestone – correcting her book proofs – and kept going until she had finished. She had seen and talked to the people that she wanted to see, her old friends, her family friends, the doctors who had become friends. Her weight was down to about 80 pounds. On Tuesday, March 11, she brought Bryan and her mother into her room (her father was at the Rothenbergs’ home uptown) and said, “Don’t give me any more liquids.” She was ready to go.
When she called her father to tell him about this decision, Bryan told me, Jon gently asked her to reconsider. But Laura, who had seemed almost detached until that point, erupted into emotion. She was firm. “Daddy, I don’t want to be here anymore. You know, I tried.” And he said, “I know you tried, Laura.”
She was weeping. “I’ve tried, I’ve tried,” she said to them all, “pleading with us to understand,” Bryan told me. “From then on, all we wanted for her was to die comfortably and quickly.” She lived for eight more days, receiving only enough fluids to take the medications that kept her comfortable and out of pain. On the morning of the eighth day, Bryan called her parents and said she seemed to be at the end. They came downtown. She asked her parents to sit at the foot of the bed and told Bryan to hold her hand. “And she looked at us – and it was like she was taking a picture,” Bryan said.
She said to Bryan, “You know, I’ll always love you – I’ll remember you always.” And he said the same, and they kissed while she was gasping for breath, and he could feel her breath coming in and out.
She had some final, private words for each of them, and then she pumped her fist in the air and cried, “Yes!” – “like she was winning a marathon,” Bryan said. There was no agony, no strain. She was gasping more and more. And then she just wanted to hold her mother’s hand. And finally, at eight o’clock in the evening on the first day of spring, Laura died.
Laura’s attitude toward her own body had always been that it was public space, never free of assaults and interventions, and there was an open casket at her wake. After the eulogies at her crowded memorial service three weeks later, there was a wild rain, thrown from the upper balconies, of origami cranes, those symbols of Laura’s indomitable hope and her love of beauty — both of which seemed astonishingly present even in her death.
The revolutionary political theorist Antonio Gramsci said that he lived by pessimism of the intellect and optimism of the will. Laura maintained that attitude most of her life – she imagined a full life for herself even as she knew that medical reality was against her. She wrote Breathing for a Living because words were always her sharpest weapon and best defense. She knew very clearly what was happening to her; she was unprotected in that regard, at her own insistence, but she had hope for the power of her own personality and made herself permanent through love and the words to describe it.
“I definitely think about after I’m gone,” she said on her last radio recording. “I’ve always been scared that people would forget about me… Years go by and you know, someone who dies isn’t the first person you think of when you wake up… But I’ll find a way so that people won’t forget about me.”