In trying to prevent suicide, we may actually abet it
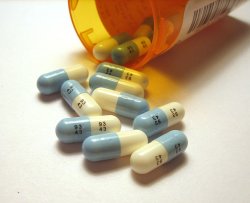
Fluoxetine HCl 20mg capsules. Photo: Tom Varco. Source: Wikimedia Commons.
Under mounting pressure, the Food and Drug Administration last week announced changes in the labeling of 10 antidepressants to reflect apprehension that they may increase suicidal feelings, especially among children and adolescents, especially in the first weeks of treatment. The issue surfaced in the early 1990’s, when the drugs — Prozac and Zoloft the most common among them — first hit the market, and was soon dismissed. But recent studies have reignited concern. The labeling change is intended to make doctors more cautious about prescribing the drugs and patients more cautious about taking them. Such vigilance is crucial. But if the labeling scares depressed people away from medications that would help them, it is also dangerous.
It is probably the case that antidepressants both cause and prevent deaths. But it is also clearly the case that they prevent more deaths than they cause. The danger is that in seeking to prevent antidepressant-related suicide, we will increase depression-related suicide.
People die from chemotherapy, but because we recognize that cancer is often fatal, we accept the risks of treatment. We tend to be less aware of the mortal nature of depression. Some 700,000 American adults attempt suicide every year; someone succeeds in committing suicide in the United States every 17 minutes. Four percent to 10 percent of people who suffer from major depression commit suicide. Untreated depression is lethal.
The solution is not to stop using the drugs, but to identify the populations in which their use could lead to suicide. There is no simple test to pinpoint those at risk. The best defense is to monitor people who are taking antidepressants — which we should do anyway. Sadly, medication has often replaced close personal attention; the best possible consequence of the labeling change would be a return to sustained scrutiny of depressed patients. (Full disclosure: my father is the chief executive of a pharmaceutical company that manufactures antidepressants.)
Depression is isolating, and part of the treatment should deal with the fearsome aloneness. Taking medication involves changing who patients are, and they need help to reassemble their own understanding of themselves. Further, responses to medication may be eccentric or unpleasant, even when not acutely dangerous, and treatment should be adjusted accordingly. For the first two months on a new medication or dosage, a qualified doctor should be keeping a close eye on the patient.
The fundamental mechanism of antidepressant suicide is not that medication aggravates depression, but that antidepressants rouse people who are in a state of glazed lethargy. The opposite of depression is not happiness, but vitality. In the depths of depression people may well lack the wherewithal to get out of bed or brush their teeth; everything seems difficult. Antidepressants are activating. There is a delicate balance between the processes by which they give energy and those by which they ameliorate despair, and sometimes the energizing comes first. When that happens, patients get the verve required for decisive action without getting the feeling that they can beat their problems. The result can be suicide. That is, a patient can go abruptly from wishing he were dead, to wanting to kill himself, to killing himself.
In addition, antidepressants may actually escalate depression in a small number of people. When we muck around with brain chemistry, we see strange and subtle effects. The emotional brain is idiosyncratic. Experiences that make one person happy — the birth of a child, the first day of spring — may drive another to despair. If events can have such diffuse consequences, so can medications. Most psychoactive drugs provoke paradoxical responses in a limited number of people: stimulants prove sedating, and sedatives make them tense. Anything that is strong enough to bring someone back from the brink of suicide is strong enough to push him there. Serotonin, the neurotransmitter affected by most of the antidepressants on the F.D.A. list, is not a simple happiness compound.
A patient should know the risks from the start. There is a world of difference between simply believing that life has no value, and knowing that feeling that way may be a side effect of medication. Patients must be able to recognize the difference. Doctors must tell them: “Look, you may have suicidal feelings on this drug. If you do, stop taking it and call me at once.” Part of what motivates suicide is the belief that things will never get better; if patients are aware that sensations are temporary, and from a specific and easily identified source, they can grapple with them.
There is work ahead. It is important to conduct studies that identify the mechanisms of antidepressant-related suicide, and to seek patterns that may predict it. Because such suicides are not frequent side effects, these studies would have to be vast, and conducted over time. Patterns of paradoxical response should be measured; imaging studies should be used to identify the basis of such responses. Studies in younger people, who seem most at risk, should be required. The pharmaceutical industry should bear at least in part the expense of such research.
“What we don’t know for sure is what is the best thing to do for a child who’s depressed,” Dr. Robert Temple of the F.D.A. said when the new labeling was announced. Depression, he said, “can be a fatal illness,” and added, “What we don’t know is whether the long-term benefits outweigh the risks.” The benefits almost certainly outweigh the risks. That doesn’t mean that we can ignore the risks.
As a society, we are overmedicated and undermedicated. Many people with severe depression go untreated, and have barren, miserable lives because of it, while others commit suicide. Only 15 percent of people with major depression get appropriate treatment. Meanwhile, people with an inflated idea of how happy we should be, who want to medicate away their personalities, take risks seeking pharmaceutical remedies to human foibles.
Both problems are authentic, but undermedication is the more dangerous. What emerges clearly from the new F.D.A. warning is that people should act with caution on both fronts. Avoid medications if they can’t help; take them if they can, but then pay attention to what happens.